Physical Therapy

Physical therapy helps you move better so you can return to daily life with less pain, more
confidence, and better control. At iMotion Physical Therapy in Fremont and San Jose, we focus on
restoring function—so you can walk, work, exercise, and handle everyday routines more
comfortably and safely. Rather than chasing quick fixes, our goal is long-term movement health
and durable results.
Movement problems rarely come from a single source. Pain, stiffness, or limited mobility can
build over time from injury, repetitive strain, altered movement patterns, or changes in
strength, flexibility, balance, or coordination. Physical therapy takes a whole-body approach to
identify what’s contributing to your symptoms and improve how your body works as a system.
At iMotion, you’ll work with a licensed physical therapist who evaluates how you move, listens
closely to your goals and concerns, and builds a personalized plan of care designed for safe,
steady progress.
What is physical therapy and why does it matter?
Physical therapy looks at how your body moves as a connected system. Rather
than focusing only on where pain is felt, it considers how strength,
mobility, flexibility, balance, coordination, and movement habits work
together.
Physical therapy is often recommended after an injury, surgery, or
diagnosis, but it can also play an important preventive role. By identifying
movement patterns or physical stressors early, physical therapy can help
reduce the risk of future strain or injury and support long-term physical
health.
This approach allows physical therapy to address not only symptoms, but also
the underlying movement factors that contribute to discomfort, limitation,
or reduced confidence with activity.
Who is physical therapy for?
Physical therapy can support people at many different stages of recovery and
activity. Some begin after an injury or surgery. Others seek care when
everyday movement starts to feel limited, inefficient, or unreliable —
whether that means difficulty walking, trouble getting up from a chair,
reduced endurance, loss of flexibility, or decreased confidence with
exercise or work tasks.
People also come to physical therapy for recurring injuries, movement
asymmetries, coordination changes, fall prevention, or guidance on returning
safely to sport or higher levels of activity.
Whether symptoms are sudden or gradual, physical therapy focuses on
understanding what’s contributing to the change and helping you move with
greater control, efficiency, and resilience.
In many cases, physical therapy can begin without a physician referral,
though insurance requirements may vary. Our team can help guide you through
that process.
What does physical therapy help with?
By improving movement quality and function, physical therapy may help with a
wide range of concerns, including:
- Back and neck pain
- Shoulder, hip, knee, and ankle pain
- Sports injuries and overuse injuries
- Tendon and ligament irritation or injury
- Recovery after surgery
- Balance issues and fall prevention
- Conditions that affect walking, strength, or coordination
Physical therapy includes multiple areas of focus, such as orthopedic,
neurologic, and pediatric care. Based on your evaluation, your physical
therapist will help guide you to the most appropriate approach for your
needs.
How does physical therapy approach recovery?
Care begins with a comprehensive movement evaluation and a detailed
conversation about your symptoms, daily challenges, and goals. This
evaluation allows your physical therapist to observe how your body moves,
identify contributing factors, and understand how movement limitations may
be affecting your daily life.
Rather than treating symptoms in isolation, physical therapy looks at how
different parts of the body work together. Strength, mobility, flexibility,
balance, and coordination are all considered when developing a plan of care.
This approach helps address contributing factors—not just the area that
hurts.
From there, your physical therapist creates a plan designed to help you
progress safely and steadily over time, adjusting as your needs, abilities,
and activity demands change.
For more details on what to expect, visit our Patient
Resources page.
What does physical therapy include?
As your plan is carried out, physical therapy often combines hands-on care
with guided exercise and movement training. Depending on your needs, your
plan may include:
- Mobility and stretching techniques
- Strengthening and stability training
- Balance and coordination work
- Functional exercises to support daily activities
- Neuromuscular reeducation to improve movement control and coordination
- Hands-on therapy, when appropriate
- Education to support long-term results
- Home exercises to reinforce progress
These components are selected and combined intentionally, based on your
evaluation and goals, and are adjusted as you improve.
How does care progress over time?
Physical therapy focuses on building lasting improvements—not just managing
symptoms. As your movement, strength, and confidence improve, your program
is progressed to match your abilities and everyday movement demands.
Your plan of care may evolve over time based on how your body responds,
changes in your goals, or new physical challenges. Physical therapy
emphasizes long-term function and independence rather than relying solely on
rest, medication, or temporary activity modifications.
Our role is to help you move more efficiently, safely, and confidently so
you can return to the activities that matter most to you.
Ready to get started?
If physical therapy feels like the right next step, scheduling an evaluation is a simple place to
start. We’ll help you determine the best path forward based on how your body moves, your goals,
and your individual needs.
You can also learn more about our orthopedic, neurologic, and pediatric physical therapy services
to find the care that best fits you.
Orthopedic Physical Therapy
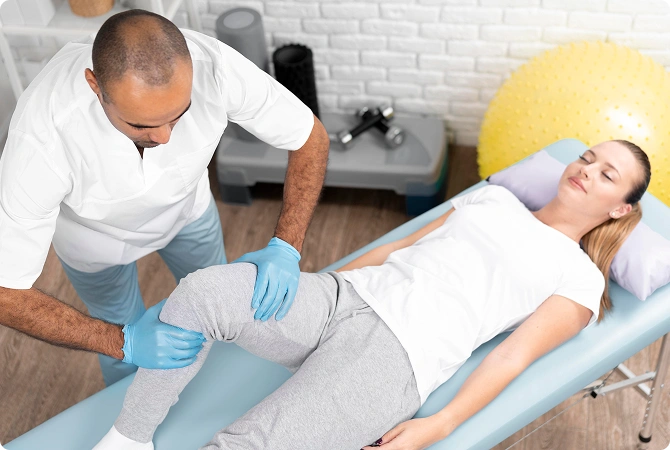
Orthopedic physical therapy focuses on conditions affecting the muscles, joints, tendons,
ligaments, and bones. It is commonly recommended after injury or surgery, but many people
also seek care for gradual-onset pain, mobility restrictions, joint instability, or
recurring flare-ups that interfere with work, exercise, or daily movement.
Rather than focusing only on where symptoms are felt, orthopedic care looks at how joints
move, how muscles support and control those joints, and how load is distributed through the
body during activity. Changes in mechanics, strength, or tissue tolerance often contribute
to irritation over time — even when imaging findings are minimal or unclear.
The goal is to restore joint mobility, improve strength and stability, rebuild tolerance to
load, and support a safe return to the activities that matter to you.
What is orthopedic physical therapy and why does it matter?
Orthopedic physical therapy focuses on the musculoskeletal system, including
muscles, joints, tendons, ligaments, and bones. Pain or movement limitations
in these areas often develop due to injury, repetitive stress, poor movement
mechanics, or changes in strength and mobility over time.
Rather than treating pain in isolation, orthopedic physical therapy looks at
how joints move, how muscles support them, and how movement patterns may be
contributing to ongoing discomfort or strain. This approach helps address
underlying movement factors and supports more durable improvements.
Who is orthopedic physical therapy for?
Orthopedic physical therapy can benefit people with both new and
long-standing
musculoskeletal concerns. Some individuals seek care after an injury or
surgery, while others come in for persistent pain, stiffness, or difficulty
performing daily or recreational activities.
If pain, stiffness, or weakness is interfering with your normal routine—or
if
certain movements feel limited, uncomfortable, or unreliable—orthopedic
physical therapy may help you move with greater ease and confidence.
What does orthopedic physical therapy help with?
Orthopedic physical therapy may help with a wide range of musculoskeletal
concerns, including:
- Back pain, stiffness, or sciatica
- Neck pain or limited range of motion
- Shoulder pain, especially with reaching or lifting
- Hip pain or difficulty walking
- Knee pain, including pain with stairs or squatting
- Foot and ankle pain or instability
- Tendon irritation and overuse injuries
- Sprains and strains
- Recovery after orthopedic surgery
Your physical therapist will help determine which movement factors are
contributing to your symptoms and how best to address them.
How does orthopedic physical therapy approach recovery?
Care begins with a comprehensive movement evaluation and a conversation
about
your symptoms, daily activities, and goals. This evaluation allows your
physical therapist to assess joint mobility, strength, movement mechanics,
and how your body responds to different tasks.
Orthopedic physical therapy emphasizes restoring efficient movement,
improving joint support, and reducing physical stress on affected areas.
Treatment is guided by how your body moves—not just where pain is felt.
From there, your physical therapist builds a plan designed to help you
improve safely and progressively over time.
What does orthopedic physical therapy include?
As your plan is carried out, orthopedic physical therapy may include a
combination of:
- mobility and stretching to improve range of motion
- strengthening to support joints and stability
- movement retraining to improve mechanics and reduce strain
- hands-on therapy, when appropriate
- education and home exercises to reinforce progress
Your program is tailored to your needs and adjusted as your movement,
strength, and confidence improve.
How does care progress over time?
Orthopedic physical therapy focuses on building lasting improvements rather
than temporary relief. As pain decreases and movement improves, your program
is progressed to support greater strength, endurance, and activity demands.
Care is adjusted based on your response, goals, and the activities that
matter most to you—whether that means returning to work, sport, or everyday
movement with less discomfort and greater confidence.
What can I expect?
Your first visit includes a movement evaluation and a discussion about your
symptoms and goals. From there, we’ll build a treatment plan designed to
help you improve safely and steadily over time.
We’ll meet you where you’re at and progress your program based on your
comfort, response to care, and goals.
For more details on what to expect, visit our Patient
Resources page.
Ready to get started?
If joint pain, stiffness, or instability is affecting your daily life, an orthopedic evaluation
can help clarify what’s contributing to the issue and what to do next. We’ll assess how your
joints and muscles are working together and create a plan tailored to your goals.
When you’re ready, we’re here to help you move forward with confidence.
Neuro
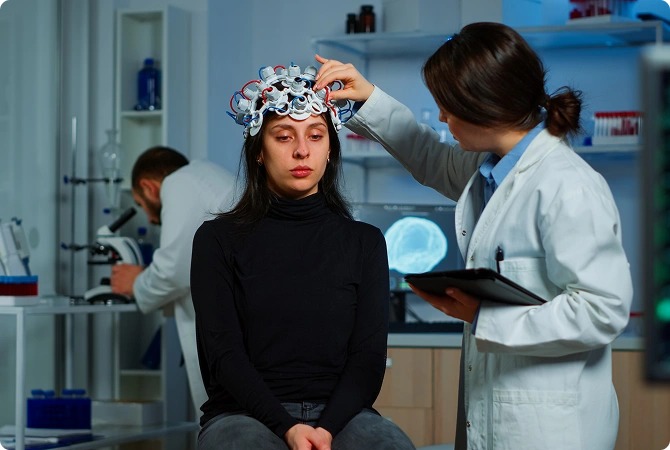
Neurologic physical therapy supports individuals whose movement, balance, coordination, or
walking have been affected by changes in the nervous system. This may include conditions such as
stroke, Parkinson’s disease, multiple sclerosis (MS), vestibular disorders (including vertigo),
or other neurologic movement changes.
When the nervous system is involved, movement may feel slower, less coordinated, less steady, or
more difficult to control. Neuro rehabilitation focuses on structured, task-specific practice to
help improve motor control, safety, and functional mobility in daily life.
Care is personalized to your goals, current abilities, and the activities that matter most to
you.
What does neurologic physical therapy help with?
Neurologic physical therapy may help with common concerns such as:
Walking and Mobility
- Changes in walking pattern or gait speed
- Difficulty navigating uneven surfaces or crowded environments
- Reduced step length or foot clearance
- Hesitation or freezing during movement
Balance and Fall Prevention
- Unsteadiness when standing or turning
- Increased fall risk
- Difficulty maintaining balance during dual-task activities
- Vestibular-related instability
Strength and Motor Control
- Muscle weakness related to neurologic conditions
- Decreased coordination or timing of movement
- Reduced endurance with activity
- Difficulty initiating or sequencing movement
Functional Independence
- Difficulty with transfers (standing up, sitting down, bed mobility, stairs)
- Slower or less efficient movement during daily tasks
- Changes in posture affecting safety or mobility
What does neurologic physical therapy include?
Your plan may include a combination of:
- Gait training and walking practice
- Balance and fall prevention training
- Strengthening and mobility exercises
- Coordination and motor control activities
- Functional task training for daily activities
- Home exercise programs to reinforce progress
- Caregiver education and home safety guidance, when appropriate
Treatment is structured, progressive, and adjusted based on your response and
evolving goals.
Parkinson’s physical therapy (including PWR!)
Physical therapy can be beneficial at all stages of Parkinson’s disease. We
provide Parkinson’s physical therapy at all iMotion locations except Lake,
based on your symptoms, mobility, and goals.
We also offer PWR! (Parkinson Wellness Recovery)-informed therapy, and we
have PWR! certified providers at our Mowry clinic.
What can I expect?
Your first visit includes a movement evaluation and a conversation about your
symptoms and goals. From there, we’ll build a treatment plan designed to
help you improve safely over time.
For more details on what to expect, visit our Patient
Resources page.
Ready to get started?
If walking, balance, or coordination changes are affecting your independence
or confidence, a neurologic evaluation can help clarify what’s contributing
and outline a clear plan forward.
When you’re ready, we’re here to support steady, meaningful progress.

Parkinson’s disease can affect walking, balance, posture, coordination, and everyday
movement. Physical therapy can help you stay active, improve safety, and maintain
independence through targeted training and progressive practice.
At iMotion Physical Therapy, we provide Parkinson’s physical therapy at all clinics except
Lake.
Why physical therapy matters with Parkinson’s
Physical therapy can be helpful at every stage of Parkinson’s disease—even when
symptoms are mild. Early on, changes in movement may be subtle, which is why a baseline
physical therapy evaluation can be valuable. Ongoing check-ins and periodic
re-evaluations can help address movement challenges as your needs change over time.
What symptoms can Parkinson’s physical therapy help with?
Parkinson’s physical therapy may help with common concerns such as:
- Smaller steps or shuffling while walking
- Freezing episodes or difficulty initiating movement
- Balance issues and fall risk
- Stiffness or tightness
- Tremors that affect movement control
- Difficulty getting up from a chair or out of bed
- Changes in posture or slower movement
- Reduced endurance or confidence with activity
What is PWR! and how can it help?
PWR! (Parkinson Wellness Recovery) and PWR!Moves are Parkinson’s-specific exercise and
movement strategies used by physical therapists to support mobility and function. PWR
training can be used in physical therapy sessions and carried over into daily routines
and activities.
At iMotion Physical Therapy, we work progressively with you—physically and
cognitively—to address your unique symptoms and goals. Everyone is an individual, and
your plan should reflect that.
PWR! certified providers (Mowry clinic)
We have PWR! certified providers at our Mowry clinic, and PWR-based care may be
incorporated into your plan when appropriate.
If you are interested in PWR!Moves specifically, we can help guide you to the right
clinic and therapist based on your needs.
What does Parkinson’s physical therapy include?
Your plan may include a combination of:
- Gait training to improve walking quality and safety
- Balance training and fall prevention strategies
- Mobility and flexibility work to address stiffness
- Strengthening and endurance training
- Movement strategies for turning, transitions, and daily activities
- Home exercises to support progress between visits
- Caregiver education and safety guidance (when appropriate)
What can I expect?
Your first visit includes a movement evaluation and a conversation about your symptoms,
daily challenges, and goals. From there, we’ll build a plan designed to support safer
movement and steady progress over time.
For more details on what to expect, visit our Patient Resources page.
Schedule a Parkinson’s physical therapy evaluation
Schedule an evaluation and we’ll help you build a plan to improve mobility, confidence,
and safety with everyday movement.
Pediatric Physical Therapy

At iMotion Physical Therapy, we provide pediatric physical therapy for children of all
ages. From infancy through the teen years, kids develop strength, coordination, balance,
and confidence through movement—and in pediatric therapy, we often use play as a powerful
tool to build these skills in a way that feels natural and engaging.
We work with children who are experiencing developmental delays, challenges meeting
milestones, coordination or balance concerns, or difficulty keeping up with daily
activities. We also support young athletes recovering from injuries by creating a safe,
encouraging environment where they can rebuild strength, improve movement, and return to
activity with more confidence.
Our sessions are structured, supportive, and designed to keep kids engaged.
What does pediatric physical therapy help with?
Pediatric physical therapy may be recommended for children who are not meeting their
milestones, as well as children who are experiencing physical challenges due to a
condition or injury affecting their musculoskeletal system.
Pediatric physical therapy can address concerns such as:
- Lack of head control at 3 months
- Head tilting and flat head at 3 months
- Delayed rolling over at 6 months
- Delayed sitting and crawling at 9 months
- Delayed standing at 1 year
- Delayed walking at 18 months
- Clumsiness and frequent falls
- Difficulty keeping up with peers at the playground
- Injury recovery and return to sports
- Strength, balance, and injury prevention for active kids
How can pediatric physical therapy help?
Pediatric physical therapy supports development and movement through personalized
assessments, therapeutic exercises, play-based activities, and parent education. The
goal is to improve motor skills, strengthen movement patterns, and support progress in
everyday routines—at home, at school, and during play.
Early support can be especially helpful when developmental concerns are present, and
therapy can also play an important role in safe recovery after injury.
What can I expect?
Your child’s first visit includes an evaluation of movement, strength, coordination,
and development. From there, we create a plan with clear goals and activities designed
to support steady progress.
For more details on what to expect, visit our Patient Resources page.
Schedule a pediatric physical therapy evaluation
If you believe your child would benefit from care, request an appointment today to
schedule a pediatric evaluation. We’ll create a plan that supports your child’s
movement, development, and confidence—so they can participate in daily activities more
comfortably.
Occupational Therapy

Occupational therapy helps you improve your ability to do everyday tasks and routines—like
getting dressed, cooking, working, caring for others, and managing the responsibilities of
daily life. The goal is to support independence and help you participate more comfortably
in the activities that matter most.
At iMotion Physical Therapy, occupational therapy is tailored to your needs and focused on
practical progress you can carry into real life.
What’s the difference between occupational therapy and physical therapy?
Both occupational therapy and physical therapy support recovery and function, but they
focus on different goals.
-
Physical therapy focuses on improving movement, strength, balance, and mobility—often
for walking, pain, and returning to activity.
-
Occupational therapy focuses on improving your ability to complete daily tasks and
routines—especially when pain, weakness, or limited hand and arm function makes
everyday activities harder.
Many people benefit from using both as part of their plan of care.
What does occupational therapy help with?
Occupational therapy may help with challenges such as:
- Difficulty with daily tasks (dressing, bathing, grooming)
- Hand, wrist, or elbow pain that affects function
- Weakness, stiffness, or limited range of motion in the upper body
- Difficulty with gripping, lifting, or fine motor tasks
- Recovery after injury or surgery that impacts daily activity
- Support with returning to work or regular routines
- Coordination or task-completion challenges that affect independence
Examples may include buttoning a shirt, opening jars, typing, cooking, lifting a bag,
or completing work tasks more comfortably. Occupational therapy can also support
individuals recovering from neurologic conditions that affect daily function.
How can occupational therapy help?
Occupational therapy focuses on helping you build skills, strategies, and confidence
for daily life. Your occupational therapist may work with you on movement training,
task-specific practice, and problem-solving approaches to make activities feel more
manageable and less painful.
What does occupational therapy include?
Your plan may include a combination of:
- Goal-based activities to improve everyday performance
- Strengthening and mobility exercises (when appropriate)
- Coordination and fine motor training
- Activity modification and movement strategies
- Education and home recommendations to support progress between visits
What can I expect?
Your first visit includes an evaluation focused on your symptoms, daily challenges,
and goals. From there, we’ll create a plan with clear goals to support steady
progress.
For more details on what to expect, visit our Patient Resources page.
Schedule an occupational therapy evaluation
Schedule an evaluation and we’ll help you feel more confident and capable in the
activities you need and want to do.
Speech Therapy (Speech-Language
Pathology)

Speech therapy helps children and adults improve communication and swallowing skills.
Speech-language pathologists (SLPs) work with people to support clearer speech, stronger
language skills, improved voice, and safer swallowing so daily life feels easier and more
confident. We work with both pediatric and adult patients, and care is tailored to your
needs and goals.
At iMotion Physical Therapy, our speech therapy services focus on practical progress you
can carry into everyday routines.
What’s the difference between speech therapy, occupational therapy, and physical
therapy?
These services often work together, but they focus on different goals:
- Physical therapy focuses on movement, strength, balance, and mobility.
- Occupational therapy focuses on daily function and independence with everyday
tasks.
- Speech therapy focuses on communication, cognitive-communication, voice, and
swallowing.
What does speech therapy help with?
Speech therapy may help with concerns such as:
- Difficulty being understood when speaking
- Speech sound challenges
- Stuttering or fluency concerns
- Voice strain, hoarseness, or vocal fatigue
- Language difficulties (understanding or expressing thoughts)
- Social communication challenges
- Cognitive-communication concerns (attention, memory, problem-solving)
- Swallowing difficulties (dysphagia), including coughing or choking with food or
liquids
Examples may include trouble finding words, difficulty being understood on the phone,
voice fatigue by the end of the day, or coughing while eating or drinking.
Speech therapy may also support individuals recovering from neurologic conditions
(such as stroke, concussion, or traumatic brain injury) when communication or
swallowing are affected.
Conditions we treat
Speech therapy can support individuals with communication or swallowing conditions such
as:
- Speech sound disorders (including articulation disorders)
- Stuttering (fluency disorders)
- Voice disorders (including hoarseness and vocal strain)
- Language disorders (expressive and receptive language)
- Cognitive-communication disorders (attention, memory, and problem-solving)
- Dysphagia (swallowing disorders)
- Neurologic speech and language changes (such as after stroke, concussion, or
traumatic brain injury)
What does speech therapy include?
Your plan may include a combination of:
- Speech and language exercises based on your needs
- Strategies to improve clarity and confidence in communication
- Voice techniques and education (when appropriate)
- Cognitive-communication training (when appropriate)
- Swallowing strategies and exercises (when appropriate)
What can I expect?
Your first visit includes an evaluation focused on your symptoms and goals. From
there, we’ll create a plan with clear goals to support steady progress.
For more details on what to expect, visit our Patient Resources page.
Schedule a speech therapy evaluation
Request an appointment today to schedule a speech therapy evaluation. We’ll help you
communicate more confidently and participate more comfortably in daily life.
Visit iBliss Wellness

iBliss Wellness is iMotion Physical Therapy’s sister company, offering wellness-focused
services that support relaxation, recovery, and overall well-being. iBliss provides
acupuncture and medical massage exclusively at our Mowry clinic in Fremont.
Wellness services through iBliss are designed to complement—rather than replace—medical
care or rehabilitation. Many people choose to incorporate these services alongside
physical therapy, exercise, or other health routines.
Wellness services offered through iBliss
- Acupuncture – commonly used to support pain relief, stress
management, and nervous system regulation.
- Medical massage – targeted massage focused on muscle tension,
recovery, and soft-tissue health.
All iBliss services are provided at our Mowry location in Fremont in a calm,
supportive environment.
Wellness services and rehabilitation services serve different—but often
complementary—roles.
- Rehabilitation services (such as physical therapy, occupational
therapy, and speech therapy) are medical services focused on evaluating, diagnosing, and
treating pain, injury, or functional limitations.
- Wellness services focus on supporting overall well-being, including
physical comfort, emotional balance, stress management, and quality of life—not just the
absence of symptoms.
Wellness care recognizes that health is multidimensional and influenced by how we move,
feel, recover, and connect in daily life. Some individuals choose to use wellness services
alongside rehabilitation care for additional support, while others use them independently as
part of an ongoing self-care routine.
disclaimer
Wellness services provided through iBliss are not a substitute for medical care.
Please consult a qualified healthcare provider for diagnosis or treatment of medical
conditions.
Acupuncture (via iBliss)
 iBliss Wellness
iBliss Wellness
Acupuncture is a wellness-based treatment rooted in traditional Chinese medicine that
involves the insertion of thin, sterile needles at specific points on the body. Today,
acupuncture is commonly used to support pain relief, stress reduction, and overall
balance.
At iBliss, acupuncture is offered as a wellness service at our Mowry clinic in Fremont to
help individuals manage discomfort, relax the body, and support recovery.
What does acupuncture help with?
Acupuncture is commonly used to support individuals experiencing:
- Chronic or intermittent pain
- Muscle tension or soreness
- Headaches or migraines
- Stress, anxiety, or nervous system tension
- Sleep difficulties
- Fatigue or low energy
- Recovery from physical strain or overuse
Many people seek acupuncture as part of a broader wellness or pain-management
routine.
How does acupuncture work?
Acupuncture is thought to influence the body’s natural regulatory systems by
stimulating specific points associated with circulation, nervous system activity, and
the body’s natural pain-relief responses. Modern research has explored acupuncture’s
role in pain modulation, relaxation, and nervous system regulation, which is why it is
commonly used as a complementary wellness service.
What can I expect during an acupuncture session?
Sessions typically begin with a brief conversation about your concerns and goals.
Treatment is performed in a quiet, relaxing setting. Sensations vary, but most people
describe treatment as comfortable and calming.
Acupuncture as part of your wellness routine
Acupuncture through iBliss is intended to support overall comfort and well-being. It
is not a substitute for medical diagnosis or treatment, but it may complement other
care when appropriate. Some individuals choose to combine acupuncture with physical
therapy or other rehabilitation services for additional support.
Disclaimer
Wellness services provided through iBliss are not a substitute for
medical care. Please consult a qualified healthcare provider for diagnosis or
treatment of medical conditions.
Medical Massage (via iBliss)
 iBliss Wellness
iBliss Wellness
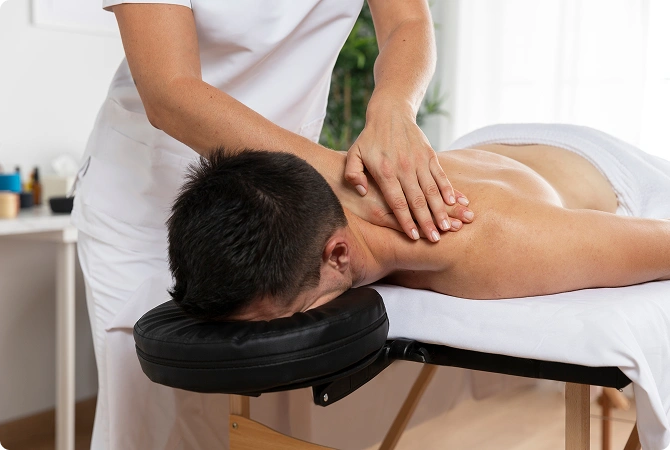
Medical massage is a targeted form of therapeutic massage focused on specific areas of
muscle tension, stiffness, or discomfort. Unlike relaxation massage, medical massage is
typically goal-oriented and tailored to individual needs.
At iBliss, medical massage is offered as a wellness service at our Mowry clinic in Fremont
to support muscle recovery, mobility, and stress reduction.
What does medical massage help with?
Medical massage may be helpful for individuals experiencing:
- Muscle tightness or chronic tension
- Postural discomfort related to daily activity or work
- Stress-related muscle pain
- Soft-tissue restrictions affecting comfort or movement
- General stiffness or fatigue
- Recovery support after exercise or physical activity
How is medical massage different from relaxation massage?
Medical massage focuses on specific problem areas rather than full-body relaxation
alone. Techniques are selected based on your comfort level and goals, with attention to
muscles that feel restricted, overworked, or tense. The goal is to support soft-tissue
health and comfort—not to diagnose or treat medical conditions.
What can I expect during a medical massage session?
Your session typically begins with a brief discussion about areas of concern.
Treatment is then tailored to those areas using appropriate pressure and techniques.
Mild soreness can occur after deeper work, but many people report improved comfort and
relaxation afterward.
Medical massage as part of your wellness routine
Medical massage through iBliss is designed to complement physical activity, stress
management, and recovery. Some individuals choose to use medical massage alongside
physical therapy or exercise programs when coordinated appropriately.
Disclaimer
Wellness services provided through iBliss are not a substitute for
medical care. Please consult a qualified healthcare provider for diagnosis or
treatment of medical conditions.
Aquatic Therapy

Aquatic therapy is a form of physical therapy performed in a heated, in-clinic pool. The
water creates a supportive environment that reduces stress on joints while still allowing
meaningful work on strength, balance, and mobility.
At iMotion Physical Therapy, aquatic therapy is available at our San Jose location and may
be incorporated into your overall rehabilitation plan when appropriate.
For some individuals, exercising in water feels more comfortable because the body is
partially supported and joints are not carrying full body weight. Movements that may feel
stiff, painful, or unstable on land often feel smoother and more manageable in water.
For others, aquatic therapy serves as an early phase of rehabilitation — allowing them to
rebuild strength, coordination, and confidence in a lower-impact setting before fully
returning to land-based exercise and daily activity.
What is aquatic therapy and why does it matter?
Aquatic therapy uses the natural properties of water — buoyancy, resistance, and
hydrostatic pressure — to support rehabilitation.
- Buoyancy reduces joint loading by partially supporting body
weight.
- Water resistance provides controlled strengthening in multiple
directions without heavy weights.
- Hydrostatic pressure offers light compression that may help
manage swelling and improve body awareness.
Because water decreases impact while still allowing resistance, it creates an
environment where exercise can continue even when traditional weight-bearing activity
feels limited.
Aquatic therapy is not separate from physical therapy. It is one therapeutic setting
within a structured plan of care.
Who may benefit from aquatic therapy?
Aquatic therapy may be appropriate for individuals who:
- Experience joint pain with walking or prolonged standing
- Are recovering from orthopedic surgery
- Have arthritis or persistent joint stiffness
- Find weight-bearing exercise uncomfortable
- Have balance concerns and feel more secure in a supported setting
- Need gradual reintroduction to exercise after injury
If strengthening or mobility work on land feels difficult, water-based therapy may
offer a more tolerable starting point.
Your physical therapist will determine whether aquatic therapy aligns with your
condition, medical history, and goals.
What does aquatic therapy include?
Aquatic therapy sessions are structured and guided by a licensed physical therapist.
Treatment may include:
- Gait training and walking in water
- Mobility and flexibility exercises
- Progressive strengthening using water resistance
- Balance and coordination training
- Low-impact cardiovascular conditioning
Exercises are progressed gradually based on your tolerance and response to care.
As strength and movement tolerance improve, aquatic therapy may be paired with — or
transitioned to — land-based physical therapy to support long-term function.
How does aquatic therapy support recovery?
Care begins with a comprehensive movement evaluation and a discussion about your
symptoms and goals. If aquatic therapy is appropriate, your therapist will integrate
water-based sessions into your overall rehabilitation program.
The goals remain consistent with all iMotion physical therapy services:
- Improve movement quality
- Restore strength and stability
- Increase activity tolerance
- Support safe, steady progress
Water provides a therapeutic environment that can make those goals more accessible for
some individuals.
Frequently Asked Questions
No. Aquatic therapy is conducted in a controlled clinical pool.
Your
therapist is present and guiding you throughout the session.
In many cases, aquatic therapy may begin once cleared by your
surgeon. Your
therapist will determine appropriate timing and progression.
No. It may be used at different stages of recovery when reduced
joint
loading improves exercise tolerance.
Aquatic therapy is structured rehabilitation directed by a
licensed physical
therapist and based on your individual evaluation and goals.
Not necessarily. Aquatic therapy may be combined with land-based
physical
therapy depending on your needs and progression.
What can I expect?
Your first visit includes a detailed movement evaluation to determine whether aquatic
therapy should be part of your care.
If appropriate, your therapist will guide you through structured pool sessions
designed to improve mobility, strength, balance, and overall function.
For more information about what to expect during care, visit our Patient
Resources
page.
Ready to get started?
If you are interested in aquatic therapy in San Jose, schedule a physical therapy
evaluation and we’ll determine whether water-based rehabilitation is the right fit
for your needs and goals.
AlterG Anti-Gravity Treadmill

The AlterG Anti-Gravity Treadmill is a specialized rehabilitation tool that allows you to walk
or run at a reduced percentage of your body weight.
Using precise body-weight support technology, the AlterG system decreases the load placed
through your hips, knees, ankles, and spine while maintaining a natural walking or running
pattern. This creates a lower-impact environment where movement can continue in a controlled,
progressive way.
At iMotion Physical Therapy, AlterG may be incorporated into your
rehabilitation plan when
appropriate based on your condition, recovery stage, and goals.
What is the AlterG treadmill and how does it work?
The AlterG Anti-Gravity Treadmill.
You wear specialized shorts that zip into a chamber around your lower body. The
treadmill then uses precise air-pressure technology to gently support part of your
body weight.
Your therapist can adjust support from 100% of your body weight down to as low as 20%,
in small 1% increments.
This allows walking or running with less stress through the lower extremities while
preserving
normal movement mechanics.
Rather than avoiding activity altogether, AlterG allows movement to continue with
adjusted loading.
Why would someone use AlterG in physical therapy?
After surgery, injury, or prolonged inactivity, full weight-bearing can feel
uncomfortable or unstable. In many cases, the challenge is not strength alone—it is
rebuilding tolerance to load .
The AlterG treadmill may allow you to:
- Practice walking earlier in recovery
- Gradually increase weight-bearing over time
- Maintain cardiovascular conditioning while healing
- Improve walking mechanics in a supported setting
- Progress toward full land-based activity step by step
For runners, AlterG may support a structured return-to-running progression by allowing
gradual increases in body-weight load. For individuals with neurologic conditions
affecting gait, it can provide repetitive walking practice in a stable and supported
environment.
For some patients, aquatic therapy may be used earlier when joint unloading is needed
in a different way. AlterG may then serve as a transition back to land-based walking
and running. Your therapist will determine which approach aligns best with your needs.
What does it feel like?
Most people describe the experience as feeling lighter—almost as if gravity has been
turned down.
You remain upright. Your legs move naturally. Your heart and lungs still work. But the
impact through your joints is reduced.
For some individuals, this makes walking possible when it previously felt limited. For
others, it functions as a bridge—helping rebuild strength and endurance before
returning fully to over-ground walking or running.
Who may benefit from AlterG rehabilitation?
AlterG may be appropriate for individuals recovering from or managing:
- Orthopedic rehabilitation after lower extremity surgery
- Joint pain affecting walking tolerance
- Stress injuries
- Neurologic conditions affecting gait
- Balance impairments
- Cardiac rehabilitation, when medically appropriate
- Deconditioning after illness or inactivity
- Gradual return to running
Whether AlterG is appropriate depends on your diagnosis, healing stage, and overall
health. Your physical therapist will determine if it aligns with your broader plan of
care, which may also include orthopedic or neurologic physical therapy services.
How is AlterG used in a treatment plan?
Care begins with a comprehensive movement evaluation. If AlterG is appropriate, your
therapist will integrate it into your plan of care rather than using it as a
stand‑alone treatment.
If AlterG is appropriate, your therapist will:
- Select a safe starting body-weight percentage
- Monitor walking or running mechanics
- Adjust load and speed gradually
- Combine treadmill work with strengthening, mobility, and balance training
AlterG is not a standalone treatment. It is one component within a structured rehabilitation
program.
As your tolerance improves, weight support is gradually reduced until you return to
full body-weight activity.
Frequently Asked Questions
No. A standard treadmill does not reduce body weight. AlterG allows controlled weight support while maintaining natural walking mechanics.
The goal is to reduce joint stress and improve movement tolerance. Individual responses vary.
No. It may be used for orthopedic, neurologic, cardiac, and general rehabilitation populations.
In many cases, yes — once cleared by your surgeon. Timing and progression are determined by your physical therapist.
No. It is typically combined with strengthening, balance training, and other functional exercises.
What can I expect?
Your first visit includes a full evaluation of strength, mobility, walking mechanics,
and goals. If AlterG aligns with your recovery plan, it may be integrated to support
gradual, structured weight-bearing progression.
For more information about what to expect during care, visit our Patient
Resources
page.
Ready to get started?
If you are interested in finding out more about our AlterG treadmill, schedule a
physical therapy evaluation and we’ll determine whether it supports your recovery and
movement goals.












